Inguinal hernia with the 3D scaffold ProFlor
 Instead of unphysiological “patches”, such as flat and motionless meshes or “plugs”, for the treatment of the degenerative damages caused by inguinal hernia disease, Prof. Amato developed a different strategy in line with the pathogenesis of the disease. It concerns the innovative concept of the ProFlor technique: a 3D dynamic compliant regenerative scaffold intended for fixation free permanent obliteration of the hernia defect. Inguinal hernia repair with ProFlor represents a surgical solution in line with the physiology of the inguinal region. Thanks to its proprietary dynamic responsivity, ProFlor promotes the regeneration of the inguinal tissue wasted by hernia disease. The development of mature nerves, muscle bundles, arteries and veins represents the finalization of the regenerative response induced by ProFlor. In summary, ProFlor represents a novel category of hernia device that encapsulates four groundbreaking concepts for the treatment of inguinal hernia: regenerative scaffold, fixation-free deployment, dynamic responsive behavior and permanent defect obliteration. Thanks to these innovative features, ProFlor is poised to be a pivotal advancement in the management of inguinal hernia.
Instead of unphysiological “patches”, such as flat and motionless meshes or “plugs”, for the treatment of the degenerative damages caused by inguinal hernia disease, Prof. Amato developed a different strategy in line with the pathogenesis of the disease. It concerns the innovative concept of the ProFlor technique: a 3D dynamic compliant regenerative scaffold intended for fixation free permanent obliteration of the hernia defect. Inguinal hernia repair with ProFlor represents a surgical solution in line with the physiology of the inguinal region. Thanks to its proprietary dynamic responsivity, ProFlor promotes the regeneration of the inguinal tissue wasted by hernia disease. The development of mature nerves, muscle bundles, arteries and veins represents the finalization of the regenerative response induced by ProFlor. In summary, ProFlor represents a novel category of hernia device that encapsulates four groundbreaking concepts for the treatment of inguinal hernia: regenerative scaffold, fixation-free deployment, dynamic responsive behavior and permanent defect obliteration. Thanks to these innovative features, ProFlor is poised to be a pivotal advancement in the management of inguinal hernia.
The treatment concept for inguinal hernia repair with the 3D dynamic regenerative scaffold ProFlor: the video shows the revolutionary features of the device
https://youtu.be/bB4wPwfIhsE
Background
Inguinal hernia is a protrusion of abdominal viscera through the muscular wall of the inguinal region. It’s a common disease which yearly afflicts millions of patients worldwide. The treatment is surgical, but to date no gold standard exists. The treatment concept of the most performed techniques is covering the herniated inguinal area, one of most mobile areas in the human body, with static flat meshes fixated with sutures or other fixation methods. Nevertheless, such treatment concept, intended to reinforce the herniated groin, doesn’t take into account nor the physiology of the inguinal area, neither the genesis of hernia disease.
At this regard, most scientific studies have focused on the effects of hernia protrusion, rather than its origins. As a result, years of surgical practice have been carried out without knowledge of the pathogenesis of the protrusion. Therefore, looks like the current hernia repair techniques are not evidence based but simply empirical treatments concepts. The frequent complications occurring after conventional prosthetic repair of inguinal hernias seem to clearly embody this incongruence.
Actually, being fixed to the inguinal musculature, these static meshes hinders the natural movements of the groin thus resulting unphysiological and causing pain. Furthermore, the biological response to such passive and motionless implants is a typical foreign body reaction characterized by uncontrolled fibrotic ingrowth producing a stiff scar plate and leading to mesh shrinkage. As a results discomfort is frequent and, in some cases, the fibrotic hardening enwraps the tiny inguinal nerves causing chronic pain. Another issue of mesh shrinkage is the decoverage of the hernia opening, prelude to recurrence.
Since the last decades of past century, Professor Amato has carried out specific studies related to functional anatomy, physiology and histology of the inguinal region with the intent to definitely unveil the roots of hernia protrusions. As a result, innovative concepts regarding the pathogenesis of inguinal hernias, aspects of which were largely unknown until have been recently unveiled. In several articles published in the world’s most important scientific journals, Professor Amato has been able to demonstrate that inguinal hernias are caused by a specific degeneration of the inguinal structures resulting from the continuous orthostatic impact of the viscera on the inguinal wall and the subsequent chronic compression. The theory of chronic visceral impact as the cause of inguinal hernias has been scientifically confirmed in Professor Amato’s recent book, “Inguinal hernia: pathophysiology and genesis of the disease.” The discovery of the causes of inguinal hernias, as highlighted in Professor Amato’s book, puts an end to centuries of ignorance about the origins of this disease. This significant discovery has paved the way for new therapeutic concepts and technologically advanced systems for the treatment of this very common pathological condition. Taking into account these evidences, Prof. Amato developed a new, updated and more physiological concept for the repair of inguinal hernia by means of a dynamic responsive device engineered in 3 D fashion like a scaffold and experimented for years in large animal model.

The multilamellar design of the 3D dynamic scaffold ProFlor
This 3D scaffold, named ProFlor, is made of the same material of conventional hernia meshes: polypropylene, owns a 3D multilamellar structure designed to move in accord with the motile impulse received from the groin musculature where is inserted.
Differently of conventional motionless flat meshes, the 3D dynamic responsive scaffold ProFlor is delivered fixation free to obliterate the inguinal defect and, in line with the physiology of the inguinal area, contracts and relaxes in harmony with the groin’s musculature. Thanks to its dynamic responsivity, ProFlor effectively contrasts the degenerative source of hernia protrusion since promotes the re-growth of the typical tissue components of the groin. This is fully coherent with the scope of a device intended to defeat the degenerative source of inguinal hernia disease. Actually, moving in harmony with the inguinal region, the 3D scaffold ProFlor attracts growth factors within its context, which, in just a few weeks, regenerate the tissues that had been dissolved by the degeneration caused by the hernia disease. Specific muscular, nervous, and vascular growth factors present in ProFlor during various post-implantation phases have been identified through a long lasting scientific research, and the results have been published in the world’s most prominent scientific journals. Newly formed vessels, muscles and nerves developed into the fabric of the hernia device embody the regenerative behavior of ProFlor.
This reason, more than a common hernia prosthesis ProFlor can be defined as a regenerative scaffold.
The ProFlor technique for inguinal hernia repair: open and laparoscopic
https://youtu.be/OKV-fglkBN4
- 100% “Tension free”: no fixation of the 3D scaffold with sutures, stitches, staples or similar is needed.
- Open approach is usually carried out in local anesthesia.
- Laparoscopic approach in general anesthesia.
- Patient is usually discharged same day of the surgical procedure.
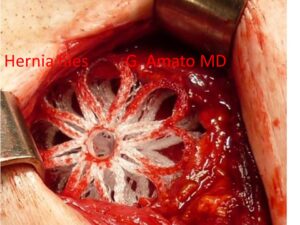
A 40 mm 3D dynamic scaffold ProFlor, evidently squeezed within the internal ring, obliterates an indirect inguinal hernia defect
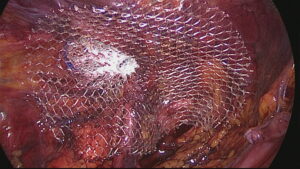 Laparoscopic image of a 40 mm sized dynamic scaffold ProFlor-E positioned into the internal inguinal ring and fully obliterating an indirect hernia defect. The flat portion of the scaffold covers the remaining posterior surface of the groin.
Laparoscopic image of a 40 mm sized dynamic scaffold ProFlor-E positioned into the internal inguinal ring and fully obliterating an indirect hernia defect. The flat portion of the scaffold covers the remaining posterior surface of the groin.
Tissue regeneration following hernia repair with the 3D scaffold ProFlor
The 3D dynamic structure of the ProFlor scaffold permanently obliterates the hernia defect, contracts and relaxes in compliance with the muscular structures of the groin. Due to its continuous movements, ProFlor acts as a regenerative scaffold for the development of new tissue components of the groin, re-establishing the inguinal barrier made of dense, viable and well vascularized tissue. The dynamic scaffold does not shrink, does not cause discomfort and postoperative pain is sharply reduced allowing the return to normal activities within few days postop.
Biologic response: 3D dynamic scaffold ProFlor vs conventional hernia meshes.
In terms of biologic response, the difference between the 3D dynamic scaffold ProFlor and the conventional meshes is noteworthy. Conventional meshes after few weeks start to produce a fibrous, hard, irregular and inelastic scar that leads to shrinkage and surface reduction of the prosthesis. This stiff scar plate, very similar to a foreign body reaction, rubbing on the inguinal floor can cause a frustrating discomfort, often complained by patients even years after surgery. The uncontrolled ingrowth of the hard scar plate, typical of conventional prostheses, is also reputed to be one of the causes of chronic pain, an event that can upset life of patients. To evaluate the differences in tissue incorporation between the two types of devices, conventional static and the 3D dynamic scaffold, Prof. Amato carried out a comparative scientific research on the biological response of the two devices in the short, medium and long-term. This scientific experience showed a manifest superiority in biologic response of the 3D dynamic scaffold ProFlor compared to conventional static meshes. The comparative scientific research demonstrated that over time the conventional flat mesh becomes a mixture of stiff scar amalgamated with amorphous synthetic material. On the contrary, the 3D dynamic scaffold ProFlor is incorporated by a well-vascularized fleshy mass that fully overwhelm its fabric, which is no more recognizable.
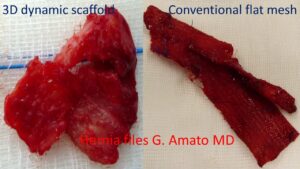
The difference of the biological response after 8 months post implantation between the 3D dynamic scaffold ProFlor, incorporated by fleshy tissue, and a conventional flat hernia mesh, deformed by a rigid scar tissue, is significant.
In the photo here on the side, the difference between the two hernia devices few months postoperative is evident. The picture shows a biopsy of the 3D dynamic scaffold and a conventional static mesh explanted for recurrence. The structure of the 3D dynamic scaffold is no longer recognizable because incorporated by a well-vascularized fleshy tissue. The other picture shows an irregularly folded conventional static mesh turned into a hardened piece of scar plate. The difference is remarkable: viable fleshy structure against a piece of hard cloth!
Quality of regenerated tissue within the structure of the 3D scaffold ProFlor
- After 3 months absence of inflammatory reaction
- Newly formed mature muscle fibers
- Plenty of nerves complete in all constituents
- Well-structured veins and arteries
- Soft and well hydrated connective
For those wishing to deepen the subject, a series of scientific articles related to these researches have been published in high ranked international scientific journals. Among the published reports, the following papers clearly summarize the regenerative features of the 3D scaffold ProFlor:
- Biologic response of inguinal hernia prosthetics: a comparative study of conventional static meshes versus 3D dynamic implants. Artif Organs. 2015 Jan;39(1)
- Neomyogenesis in 3D dynamic responsive prosthesis for inguinal hernia repair. Artif Organs. 2018 Dec;42(12):1216-1223
- Neo-nervegenesis in 3D dynamic responsive implant for inguinal hernia repair. Qualitative study. International Journal of Surgery Volume 76, April 2020, Pages 114-119
- Enhanced angiogenesis in the 3D dynamic responsive implant for inguinal hernia repair ProFlor Artificial Organs. 2021;45:933–942.
- A regenerative 3D scaffold for inguinal hernia repair. MR imaging and histological cross evidence. Qualitative study International Journal of Surgery 2021, 96, 106170
- Dynamic Responsive Inguinal Scaffold Activates Myogenic Growth Factors Finalizing the Regeneration of the Herniated Groin. J Funct Biomater. 2022 Nov 18;13(4):253
- Physiologic Cyclical Load on Inguinal Hernia Scaffold ProFlor Turns Biological Response into Tissue Regeneration. Biology, 2023, 12(3), 434
OTHER INNOVATIVE SOLUTIONS DEVELOPED BY PROF. AMATO FOR THE TREATMENT OF VENTRAL AND INCISIONAL HERNIAS
Prof. Amato also invented the tentacle shaped implant for the treatment of 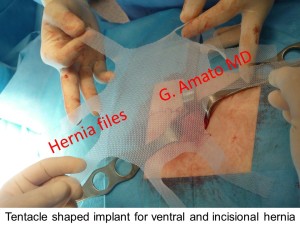 abdominal wall hernias (incisional, umbilical, epigastric and Spigelian hernias). The related surgical technique allows a fixation free surgical procedure for the treatment of these widespread pathologies. Small skin incisions, minimized surgical trauma and sharply reduced postoperative complications are the highpoints of the surgical technique. This is possible thanks to the proprietary design of the prosthesis whose elongated straps at the edges of the implant, inserted through the abdominal wall musculature, allow a permanent fixation free positioning of the implant, using the principle of tissue friction.
abdominal wall hernias (incisional, umbilical, epigastric and Spigelian hernias). The related surgical technique allows a fixation free surgical procedure for the treatment of these widespread pathologies. Small skin incisions, minimized surgical trauma and sharply reduced postoperative complications are the highpoints of the surgical technique. This is possible thanks to the proprietary design of the prosthesis whose elongated straps at the edges of the implant, inserted through the abdominal wall musculature, allow a permanent fixation free positioning of the implant, using the principle of tissue friction.
The modern prosthetic devices and the innovative surgical techniques developed by Prof. Amato allowed for significant decrease of postoperative complications. These techniques have been scientifically validated by numerous articles published in the most important scientific journals.
- Prosthetic stap system for simplified ventral hernia repair: results of a porcine experimental model. Hernia 2010;14:389-95
- A new shape of mesh to simplify and standardize the implantation procedure in ventral hernia repair. Hernia 2010;14:S-43
- Fixation free open ventral hernia repair using a new mesh with integrated placement straps. Hernia 2011;15:S21
- New mesh shape and improved implantation procedure to simplify and standardize open ventral hernia repair. A preliminary report. Hernia 2011;5:659–665
- Fixation free prosthetic repair of large umbilical hernia granting a broad defect overlap. Hernia 2012;16: Sl43-S240
- Fixation free incisional hernia repair with a newly designed mesh with integrated bands. Hernia 2012;16 (Suppl 1): 569-572
- Fixation free prosthetic repair of large umbilical hernia Hernia (2013) 17 (Suppl 2): S1-S26
- Long-term results of fixation free incisional hernia repair using a tentacle shaped implant. Surg. Technol. Int. 2017 Jul 25;30:175-181.
- Fixation free incisional hernia repair in the elderly: our experience with a tentacle-shaped implant. Aging clinical experimental research. Aging Clin. Exp. Res.2017 Feb;29(Suppl 1):173-177
- Long-term results of fixation-free incisional hernia repair with a tentacle-shaped implant. Hernia (2018) 22 (Suppl 1):S115
- Tentacle‑shaped mesh for fixation‑free repair of umbilical hernias. Hernia. 2019 Aug;23(4):801-807
- Fixation-free incisional hernia repair with tentacle-shaped implant: The results of a long-term follow up. Hernia (2019) 23 (Suppl 2):S240
- Tentacle Mesh for Fixation-Free Spigelian Hernia Repair: Mini-Invasive Approach Granting Broad Defect Overlap Journal of Clinical Medicine, 2023, 12(12), 3866
